Whiplash injuries are most commonly associated with motor vehicle collisions (MVC), although they can happen from anything that results in a sudden movement of the head—from slip and fall injuries, carnival rides, sports-related injuries, and more. When associated with MVCs, the terms “acceleration/deceleration injury” or “whiplash associated disorders (WAD)” are often applied, depending on the direction of the collision. When the striking vehicle rear-ends the target vehicle, the term “acceleration/deceleration injury” is used. WAD encompasses all scenarios and also includes the type and extent of injury. The degree of injury has been broken down into four main categories with the least amount of injury = WAD I, and the worst soft tissue injury category as WAD III. Fractures are covered separately in the WAD IV category. It has been found that the more severe the soft tissue injury (WAD III > WAD II > WAD I), the worse the prognosis, or the greater the likelihood of long-term injury-related residual problems.
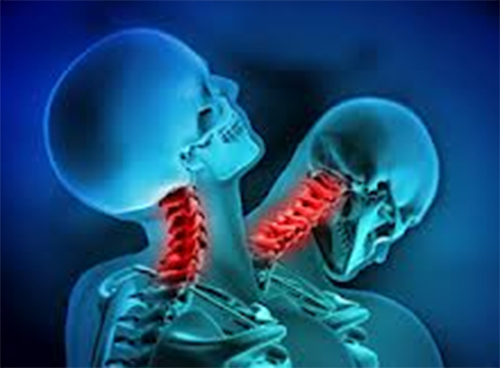
We are often asked why the neck is so vulnerable to injury in a MVC. The simple answer is the head, which weighs about 12-15 pounds (~5-7 kg), is supported by the neck and not all necks have the same length, strength, and mass. This is the reason women (especially those with longer, thin necks) are most vulnerable to the forces that occur in a WAD injury. Another reason whiplash injury can occur is the relatively “slow” speed at which we can voluntarily contract our muscles (>600 msec.) vs. relatively fast speed at which a typical rear-end collision takes to move the head on the neck during whiplash (~300 msec.)! Though the whiplash time duration will vary somewhat, depending on the speed of the collision, angle of the seat back, the distance between the head and the headrest, the “springiness” of the seat back, the weight of the two vehicles, the slipperiness of the road, if the brakes are locked, (…AND MORE!), here’s a typical breakdown of what takes place in a rear-end collision (within a 300 millisecond “typical” time frame):

The degree of injury is affected by all the items previously listed above and more. For example, if the headrest is more than two inches (~5 cm) away from the back of the head, and/or if “ramping” occurs and the head “misses” the headrest, hyper-extension can result and the soft tissues in the front of the neck can become over-stretched and/or the back of the neck can become over-compressed. Or if the rebound phase into flexion exceeds the tissue capacities, the back part of the neck can become over-stretched and the front part over-compressed.
We realize you have a choice in whom you consider for your health care provision and we sincerely appreciate your trust in choosing our service for those needs. If you, a friend, or family member requires care for Whiplash, we would be honored to render our services.